Stem Cell Therapy FAQ
Like any medical treatment, stem cell therapy has potential side effects. The specific side effects that can occur depend on several factors, including the type of stem cells used, the way they are administered, and the individual patient's health status. Some of the potential side effects of stem cell treatment include: Infection: There is a risk of infection whenever a patient undergoes any kind of medical treatment, including stem cell therapy. Rejection: If the stem cells used for treatment come from a donor, there is a possibility that the patient's immune system may recognize the cells as foreign and reject them. Tumor formation: There is a theoretical risk that stem cell therapy could lead to the formation of tumors, although this has not been observed in clinical trials. Bleeding: If the stem cells are injected into the bloodstream, there is a risk of bleeding. Pain and swelling: Injection of stem cells into certain tissues may cause pain and swelling. Immune reactions: Stem cells may trigger an immune reaction in some patients, causing inflammation or other symptoms. It's important to note that the vast majority of patients who undergo stem cell therapy experience no serious side effects. However, it's always important to discuss the potential risks and benefits of any medical treatment with a qualified healthcare provider.
Like any medical treatment, stem cell therapy has potential side effects. However, the type and severity of the side effects can vary depending on the type of stem cells used, the method of administration, the patient's medical history and health status, and other factors. Some of the potential side effects of stem cell therapy include: Tumorigenicity: There is a theoretical risk that stem cells could form tumors or other abnormal tissue growths if they are not properly controlled or differentiated. Immunogenicity: In some cases, the patient's immune system may recognize the stem cells as foreign and mount an immune response that could lead to inflammation, tissue damage, or rejection of the cells. Infection: If stem cells are administered intravenously or directly into a tissue, there is a risk of infection. Bleeding: If stem cells are administered via injection or infusion, there is a risk of bleeding at the injection site. Pain and discomfort: Some patients may experience pain or discomfort at the site where the stem cells are administered. Allergic reaction: In rare cases, patients may have an allergic reaction to the stem cells or other materials used during the treatment. It's important to note that many of these potential side effects are rare and that stem cell therapy has been shown to be safe and effective for a range of medical conditions. However, it's always important to discuss the potential risks and benefits of any medical treatment with a qualified healthcare provider.
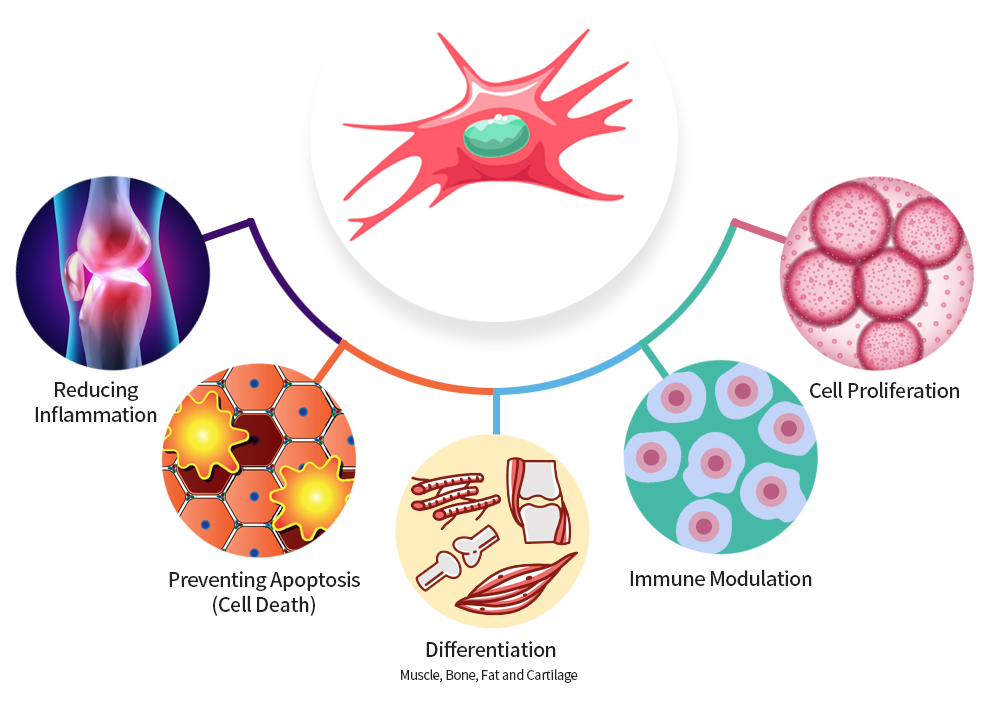
Stem cells are being investigated for their potential use in regenerative medicine and cell-based therapies to treat a wide range of diseases and conditions. Stem cell treatment involves the use of stem cells to replace or repair damaged or diseased tissues and organs in the body. There are several ways in which stem cells may work in treatment: Stem cells can differentiate into specialized cells: Stem cells can differentiate into various cell types in the body, such as nerve cells, muscle cells, and blood cells. In stem cell treatments, stem cells can be directed to differentiate into specific cell types needed to replace damaged or lost cells. Stem cells can promote tissue repair: Stem cells secrete growth factors and other molecules that can stimulate tissue repair and regeneration. These molecules can help to reduce inflammation and promote the growth of new blood vessels, which can help to repair damaged tissues. Stem cells can modulate the immune system: Stem cells have immunomodulatory properties, which can help regulate the immune system and prevent rejection of transplanted cells. This can be beneficial in autoimmune disorders or in cases where the immune system may attack transplanted cells. Stem cells can deliver targeted therapies: Stem cells can be engineered to produce and deliver therapeutic agents directly to diseased tissues or tumors. This can be a targeted approach to treat specific diseases or conditions. Stem cell treatments are being investigated for a range of conditions, including diabetes, heart disease, neurological disorders, and autoimmune diseases. While some stem cell therapies have shown promising results in preclinical studies and early clinical trials, more research is needed to fully understand their safety and efficacy in humans.
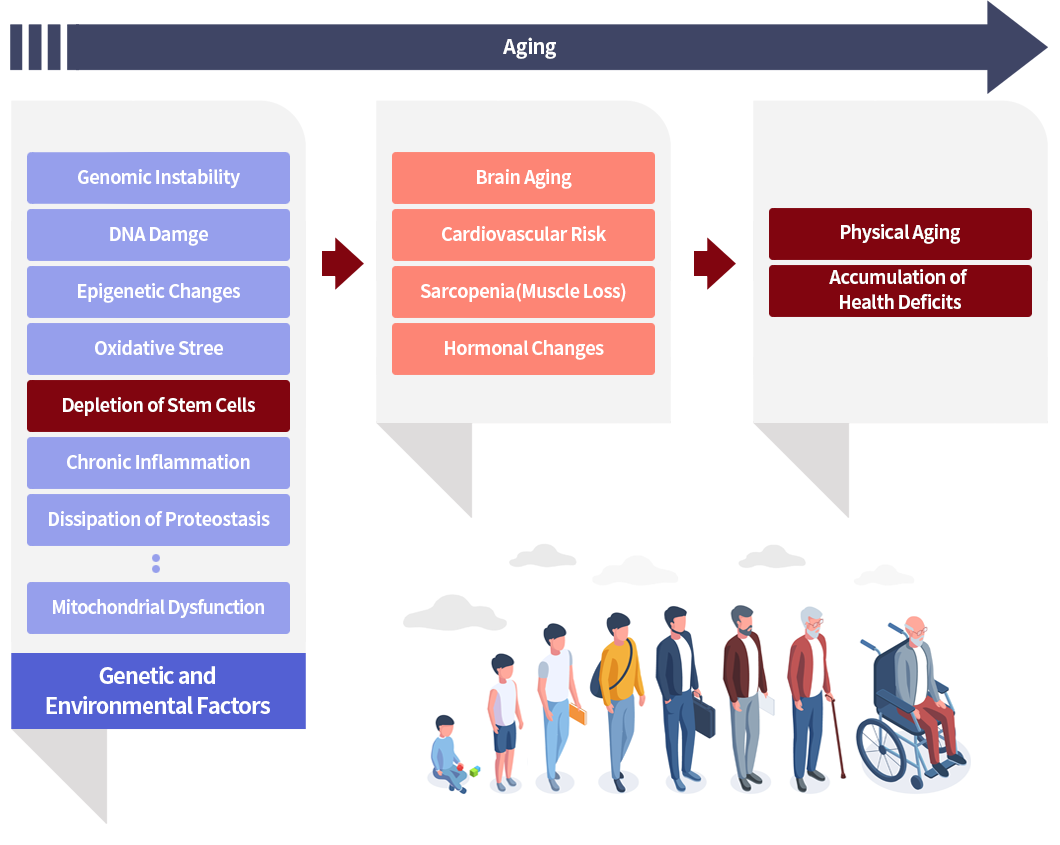
While stem cells hold great promise for treating a wide range of medical conditions, there is currently no scientific evidence to support the idea that they can prevent aging. Aging is a complex biological process that involves a combination of genetic, environmental, and lifestyle factors. Stem cells may have the ability to repair and regenerate damaged tissues, but they cannot address all of the underlying causes of aging. That being said, there is ongoing research into the potential of stem cells to slow down or even reverse some aspects of aging. For example, some studies have shown that introducing young stem cells into older animals can improve their cognitive function, reduce inflammation, and increase lifespan. Other research has explored the potential of stem cells to regenerate tissues that are affected by aging, such as the skin and muscles. While these studies are promising, much more research is needed to fully understand the role of stem cells in aging and to develop safe and effective therapies. It's important to note that aging is a natural and inevitable process, and while we may be able to delay some aspects of it, it is unlikely that we will be able to completely prevent it.
There is a possibility that your body could reject mesenchymal stem cells (MSCs) if they are not a good match for your immune system. However, the risk of rejection is generally low for several reasons: MSCs have low immunogenicity: MSCs have been found to have low levels of the molecules on their surface that can trigger an immune response, making them less likely to be recognized as foreign by the immune system. MSCs have immunomodulatory properties: MSCs have the ability to suppress immune responses, which can reduce the likelihood of rejection. They can also modulate the immune system to promote healing and tissue regeneration. MSCs can be obtained from the patient's own tissues: MSCs can be harvested from a patient's own bone marrow, adipose tissue, or other sources, reducing the risk of rejection. MSCs can be genetically modified: Researchers are investigating ways to modify MSCs genetically to make them less likely to be recognized as foreign by the immune system. However, it's important to note that there is still a risk of rejection, especially if the MSCs are obtained from a donor who is not a good match for the patient's immune system. To minimize this risk, doctors may use a matching system similar to that used for organ transplants to find a suitable donor. Additionally, patients may be given immunosuppressive drugs to reduce the risk of rejection.
12. Which one is better to use for the stem cell treatment between umbilical cell and Mesenchymal stem cell? Both umbilical cord stem cells and mesenchymal stem cells have shown promise in the field of regenerative medicine, but the best type of stem cell to use for a particular treatment depends on the specific medical condition being addressed and other factors such as the age and health status of the patient. Umbilical cord stem cells, also known as cord blood stem cells, are obtained from the blood left in the placenta and umbilical cord after a baby is born. These cells have the ability to differentiate into many different types of cells and can be used to treat a range of conditions such as blood disorders, immune system disorders, and some genetic diseases. Mesenchymal stem cells (MSCs) are a type of adult stem cell that can be found in many tissues in the body, including bone marrow, adipose tissue, and the umbilical cord. These cells have the ability to differentiate into bone, cartilage, muscle, and other types of cells. They have been studied for their potential to treat conditions such as osteoarthritis, autoimmune disorders, and spinal cord injuries. In general, the choice between umbilical cord stem cells and MSCs for a particular treatment depends on the specific medical condition and other factors such as the age and health status of the patient. For example, umbilical cord stem cells may be preferred for the treatment of certain blood disorders, while MSCs may be more suitable for treating conditions that involve tissue repair or regeneration. Ultimately, the decision of which type of stem cell to use should be made by a qualified medical professional after careful consideration of all factors.
Stem cells are unique in their ability to transform into many different types of cells in the body. This means they can be used to replace damaged or diseased cells and tissues, leading to healing and regeneration. When stem cells are introduced into an area of the body that has been damaged, they can migrate to the site of injury and begin to differentiate, or transform, into the specific type of cell needed to repair the damage. For example, if the damage is in the liver, stem cells can differentiate into liver cells; if the damage is in the heart, stem cells can differentiate into heart cells. Stem cells can also secrete growth factors and other molecules that promote tissue repair and regeneration. These factors can stimulate the growth of new blood vessels, reduce inflammation, and encourage the growth and differentiation of existing cells. In addition, stem cells can help regulate the immune system. By suppressing the immune response, they can reduce inflammation and prevent further damage to tissues. Overall, the ability of stem cells to differentiate into different types of cells, secrete growth factors, and regulate the immune system make them powerful tools for healing and regeneration in a wide range of medical conditions.
Aging frailty is a condition characterized by a decline in physical and cognitive function that can occur in older adults. Mesenchymal stem cell (MSC) therapy has been investigated as a potential treatment for aging frailty, as MSCs have the potential to regenerate damaged tissues and modulate immune function. One approach that has been investigated is the use of MSCs to treat age-related sarcopenia, which is the gradual loss of muscle mass and strength that occurs with aging. A study published in the journal Stem Cells Translational Medicine in 2018 found that a single infusion of MSCs improved muscle mass and strength in older adults with sarcopenia. The MSCs were obtained from umbilical cord tissue and were shown to secrete factors that promoted muscle regeneration and reduced inflammation. Another potential application of MSC therapy for aging frailty is in the treatment of age-related immune dysfunction. MSCs have been shown to modulate immune function and reduce inflammation, which may be beneficial in older adults with age-related immune dysfunction. A study published in the journal Stem Cells Translational Medicine in 2017 found that MSC therapy improved immune function and reduced inflammation in older adults with frailty. While the use of MSC therapy for aging frailty is still in the experimental stage, these and other studies suggest that it has the potential to be a promising treatment option for this condition. However, more research is needed to fully understand the safety and effectiveness of MSC therapy for aging frailty, and to determine the optimal sources, doses, and delivery methods of MSCs for this application.
Mesenchymal stem cells (MSCs) can be found in many tissues in the body, including fat and skin. The telomere length of MSCs can vary depending on a number of factors, including the age of the individual, the tissue source of the MSCs, and the type of culture conditions used to grow the cells. Research has suggested that MSCs from certain sources, such as umbilical cord tissue, may have longer telomeres compared to MSCs from other sources such as bone marrow or adipose tissue. However, there is still much that is not yet fully understood about the telomere length of MSCs from different tissue sources. That being said, some studies have suggested that MSCs from adipose tissue may have longer telomeres compared to MSCs from other sources. For example, a study published in the journal Stem Cells and Development in 2017 found that MSCs derived from human adipose tissue had longer telomeres compared to MSCs derived from bone marrow. It's important to note, however, that telomere length is just one of many factors that can influence the properties and behavior of MSCs. Other factors, such as the purity of the cell population, the culture conditions used to grow the cells, and the age and health status of the donor, can also impact the properties and behavior of MSCs.
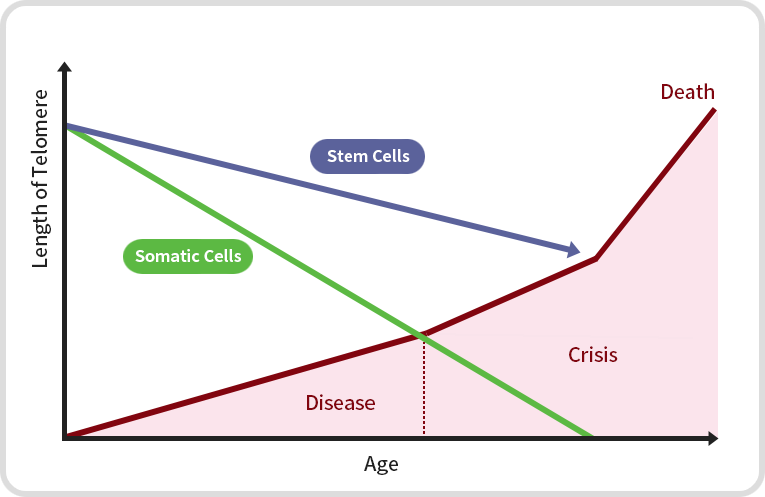
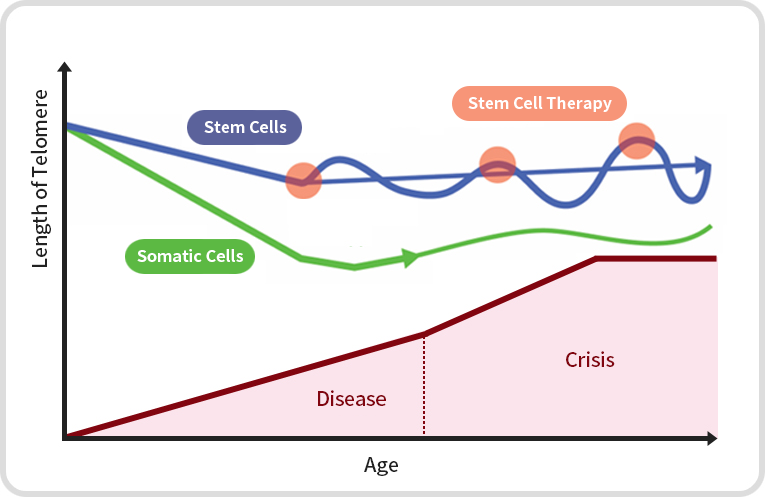
Telomeres are the protective caps at the end of chromosomes that help maintain the stability and integrity of our genetic material. Every time a cell divides, the telomeres shorten, eventually leading to cell death or senescence. As we age, our telomeres gradually become shorter, and this has been proposed as a potential mechanism for aging. Shorter telomeres have been associated with an increased risk of age-related diseases such as cardiovascular disease, diabetes, and cancer, as well as a decreased lifespan. However, it's important to note that telomere length is just one of many factors that contribute to the aging process, and the relationship between telomere length and aging is not yet fully understood. While there is evidence to suggest that telomere shortening plays a role in aging and age-related disease, it's likely that other factors such as oxidative stress, inflammation, and DNA damage also contribute to the aging process. Researchers are continuing to study the relationship between telomere length and aging in order to better understand the mechanisms of aging and develop potential interventions to slow or reverse the aging process. Telomeres are the protective caps at the end of chromosomes that help maintain the stability and integrity of our genetic material. Every time a cell divides, the telomeres shorten, eventually leading to cell death or senescence.
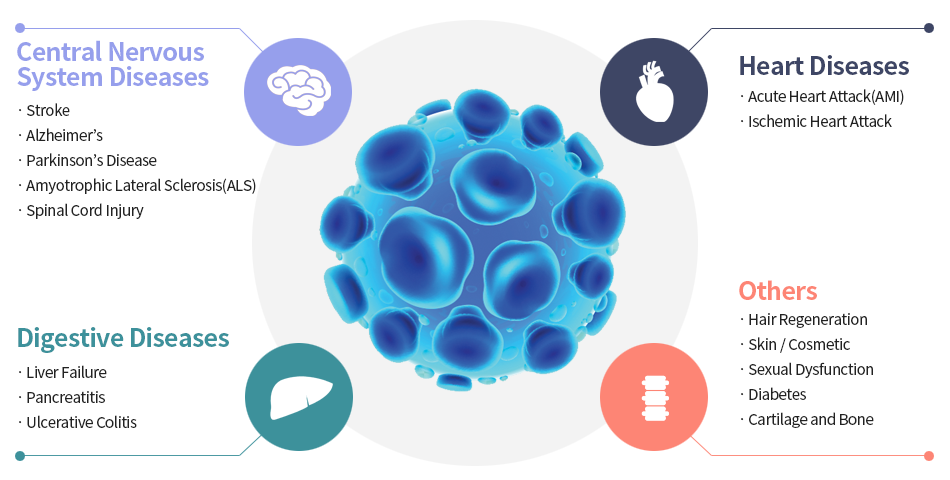
The effect of stem cell treatment can vary depending on the type of stem cells used and the specific condition being treated. In general, stem cell treatments are being investigated as potential therapies for a wide range of conditions, including heart disease, neurological disorders, autoimmune diseases, and certain types of cancer. The potential effects of stem cell treatment can include: Tissue regeneration: Stem cells have the ability to differentiate into various cell types, which can potentially allow them to regenerate damaged or diseased tissues. Anti-inflammatory effects: Some types of stem cells can secrete anti-inflammatory molecules, which can help to reduce inflammation and promote healing. Immune system modulation: Stem cells can interact with the immune system, potentially helping to modulate immune responses and reduce the risk of autoimmune reactions. Improved circulation: Stem cells have been shown to enhance blood flow to damaged tissues, which can improve healing and tissue repair. While stem cell treatments show great promise, it's important to note that many potential therapies are still in the experimental stage, and more research is needed to fully understand their safety and effectiveness. Stem cell treatments should only be undertaken under the guidance of a qualified healthcare professional.
Cytokines are a type of signaling molecule that are produced by various cells in the body, including immune cells, to regulate the immune response and other physiological processes. They are small proteins that act as messengers, transmitting information between cells to coordinate immune responses and other biological activities. Cytokines can act on specific receptors on the surface of target cells, triggering a cascade of intracellular signaling events that lead to changes in gene expression and cellular behavior. Different cytokines have different functions, ranging from promoting inflammation and cell proliferation to inhibiting the immune response and inducing cell death. Cytokines play a critical role in regulating the immune response, as they are involved in the activation, proliferation, and differentiation of immune cells, such as T cells, B cells, and natural killer cells. They also play a role in the development and maintenance of tissues and organs, such as bone and skin, and are involved in wound healing, tissue repair, and regeneration. However, dysregulated cytokine production or activity can also lead to various diseases, such as autoimmune disorders, allergies, and cancer. Therefore, cytokines are important targets for therapeutic intervention, and drugs that modulate cytokine activity are used to treat a range of diseases, including rheumatoid arthritis and certain types of cancer.
The secretome refers to the entire set of molecules secreted by cells, including proteins, lipids, nucleic acids, and other small molecules. It includes molecules that are released from the cell through various mechanisms, such as exocytosis, shedding of membrane-bound vesicles, and diffusion across the cell membrane. The secretome is important for cell-to-cell communication and plays a critical role in various biological processes, including immune regulation, tissue repair and regeneration, and tumor progression. The molecules in the secretome can act as signaling molecules, influencing the behavior of neighboring cells and tissues. In the context of regenerative medicine, the secretome of stem cells has received particular attention due to its potential therapeutic applications. Mesenchymal stem cells (MSCs), for example, are known to secrete a wide range of bioactive molecules, including growth factors, cytokines, and extracellular matrix components, which can promote tissue repair and regeneration. The use of MSC secretome as a potential therapy is being investigated as an alternative to direct stem cell transplantation, as it may provide similar therapeutic effects with lower risks and complications. Overall, the secretome is an important concept in biology and medicine, as it represents a complex and dynamic network of molecular interactions that govern cell behavior and tissue function.
Exosomes are small extracellular vehicles that are released by cells into the extracellular space. They are typically 30-150 nanometers in size and contain various molecules, including proteins, lipids, and nucleic acids such as microRNAs. Exosomes are believed to play a role in cell-to-cell communication, as they can transfer their cargo to recipient cells and influence their behavior. Exosomes are formed within multivesicular bodies (MVBs) in the cell, which are membrane-bound compartments that contain smaller vesicles. The MVBs can either fuse with the plasma membrane and release their contents into the extracellular space, or they can be degraded by the lysosome. Exosomes are released by various cell types, including immune cells, stem cells, and cancer cells, and they have been found in various bodily fluids, such as blood, urine, and saliva. They have been shown to play a role in various biological processes, including immune regulation, tissue repair, and tumor progression.
Mesenchymal stem cells (MSCs) are a type of adult stem cell that can be found in many tissues in the body, such as bone marrow, adipose tissue, and umbilical cord tissue. These cells can differentiate into a variety of cell types, such as bone, cartilage, muscle, and fat cells. MSCs are also known for their ability to modulate the immune system, which makes them potentially useful in regenerative medicine and tissue engineering. They secrete a variety of bioactive molecules that can promote tissue repair, reduce inflammation, and enhance the growth and survival of other cells. Because of these properties, MSCs are being investigated as a potential therapy for a range of conditions, including arthritis, heart disease, neurological disorders, and autoimmune diseases. However, more research is needed to fully understand their potential and how best to use them in clinical applications.